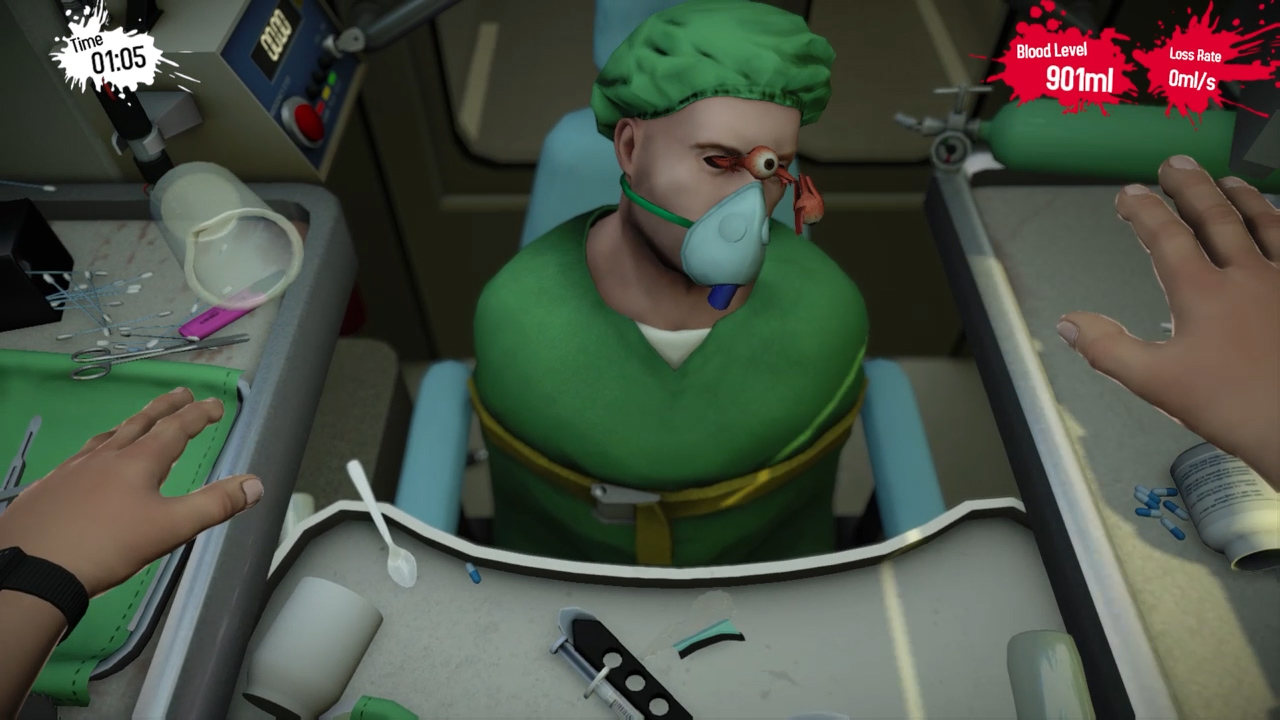 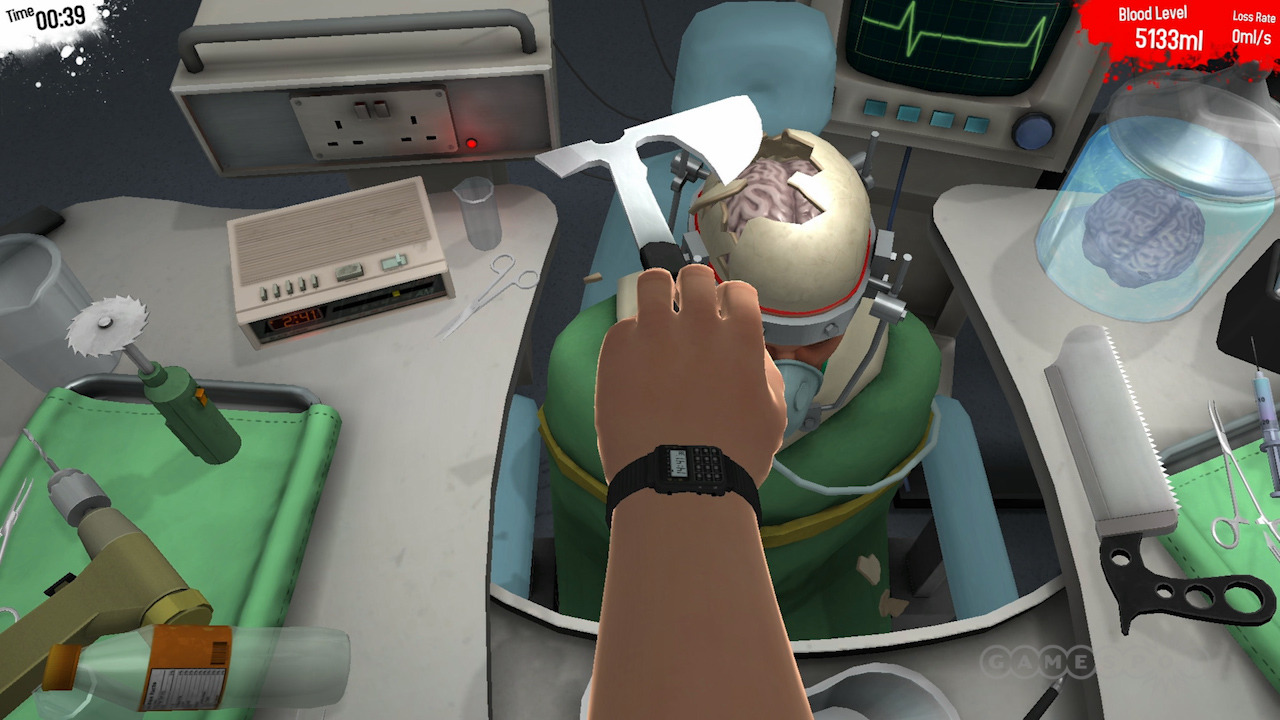
The “SOR” task ensured that participants simultaneously used the right controller as a 30° scope and the left controller as a grasper. To measure procedural complex skills, VR laparoscopic cholecystectomy was performed with three repetitions per participant. Each exercise was repeated two to eight times, depending on the need. Regarding basic skills, all participants underwent a total of 48 simulator tasks. As a basic task “scope orientation 30° right-handed” (SOR) camera navigation using the LapX-Hybrid/VR (Epona Medical B.V., Rotterdam, Netherlands) was chosen for complex skill assessment “cholecystectomy dissection” (CD) using the LapSim simulator (Surgical Science, Gothenburg, Sweden). Furthermore, a member of the study team was present during each practice session to assist in handling the simulator. īefore training, each participant received standardized information using the simulator as well as a curriculum handout with description of each exercise ensuring similar baseline. Participants in the TG underwent a two-week evidence-based, structured and validated curriculum training with different simulator tasks and increased levels of difficulty/and complexity. A positive impact, even under the current pandemic situation, allowing safe and successful surgical simulator training, may improve surgical education in diverse circumstances. The aim of our study was to evaluate the effects of VSA on skills and performance of surgical novices during a structured VR simulator training over 9 days, focusing on training process and VSA progression along the initial learning curve. However, evidence correlating the surrogate parameter VSA to surgical technical skills is limited and inconsistent, and the complexity of observed tasks has not been fully examined. Other studies have also reported a positive correlation between VSA and improved surgical performance in complex surgical tasks, such as knot tying or laparoscopic camera navigation (LCN). 
Concerning open surgery, VSA correlated positively with surgical performance, particularly during complex surgical tasks. In this context, VSA- the two-dimensional to three-dimensional conversion ability- seems to predict future surgical skills. Previous research showing correlations between innate cognitive and perceptual motoric abilities or aptitudes and surgical technical skills. To select surgical users and provide them with improved training conditions, research has focused on the identification and consideration of predictive ability parameters. In times, surgical techniques are becoming increasingly difficult the optimal training of medical novices and the selection of qualified candidates are relevant components in medical education. In this context, surgical simulation using virtual reality (VR) is a useful tool in surgical training programs which enable a safe, repeatable, patient saving and cost-effective approach outside the OR. To address this problem MIS training centers offer young surgeons the opportunity to acquire basic surgical skills prior to their first laparoscopic surgical experience. However, during residency training, limited surgical capacities and growing public concern for medical errors precludes many residents from practical exposure on actual patients, which has been further heightened during the COVID-19 pandemic, consequently reducing training opportunities. The development of these skills requires extra training time and practice. However, learning to perform and manage laparoscopic procedures is associated with additional difficulties for trainees and requires a set of psychomotor abilities differing substantially from those needed for conventional open surgery (improved hand-eye coordination, change from three-dimensional to a two-dimensional view, altered tactile and haptic feedback, etc.). Over the past decade, minimally invasive surgery (MIS) has modernized surgical care and revolutionized the face of surgery. The enforced interruption of elective surgical activities has further reduced the already limited valuable training time for surgical trainees and residents and affected the practice of basic surgical skills in the operating room (OR). COVID-19 pandemic has globally impacted patient care as well as all forms of medical education, above all training involving manual techniques and surgical training programs.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
